Pregnant women are advised against keeping cats because of the fear of contracting toxoplasmosis from cats. Toxoplasmosis is a parasitic disease caused by Toxoplasma gondii, a common parasite. Cats are its primary host, and it is a globally distributed zoonotic infectious disease.
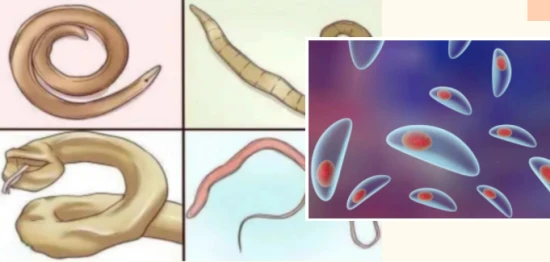
Transmission methods and harms of Toxoplasma gondii
Toxoplasmosis can be transmitted through cat feces. If a pregnant woman becomes infected while cleaning cat litter, the pathogen can be transmitted to the fetus through the placenta. Infection during the first trimester can cause severe damage to the fetal central nervous system, potentially leading to fetal death. Infection during the second trimester can cause hydrocephalus, intellectual disability, psychomotor retardation, blindness, and brain calcification in the infant. However, infection during the last trimester is most common, potentially causing retinochoroiditis and other eye damage in the infant. Damage to the central nervous system and latent asymptomatic infections can ultimately lead to disease.
Toxoplasmosis testing items
Toxoplasmosis is the first letter of TORCH, a testing method related to prenatal and postnatal care. TORCH is an acronym for a group of pathogenic microorganisms, where T (Toxoplasma gondii, Toxo) represents Toxoplasma gondii, R (rubella virus, RV) represents rubella virus, C (cytomegalovirus, CMV) represents cytomegalovirus, H (herpes simplex virus, HSV) represents herpes simplex virus, and O (others) refers to other related viruses such as Epstein-Barr virus (EBV), human immunodeficiency virus (HIV), and human parvovirus B19. Infection of pregnant women with these pathogens in early pregnancy can potentially lead to premature birth, miscarriage, intrauterine growth retardation, birth defects, stillbirth, and neonatal death.

Differential diagnosis between recent and past Toxoplasmosis infections
After infection with Toxoplasma gondii, the human body generally develops protective immunity. This immunity typically occurs in the order of specific IgM antibodies followed by IgG antibodies, with specific IgG antibodies peaking 2-5 months after the onset of clinical symptoms. Simultaneously, antibody affinity gradually increases as the immune response progresses. Recent infections show low IgG antibody affinity, while past infections show high IgG antibody affinity. Therefore, antibody affinity testing can be used to differentiate between recent and past infections.


